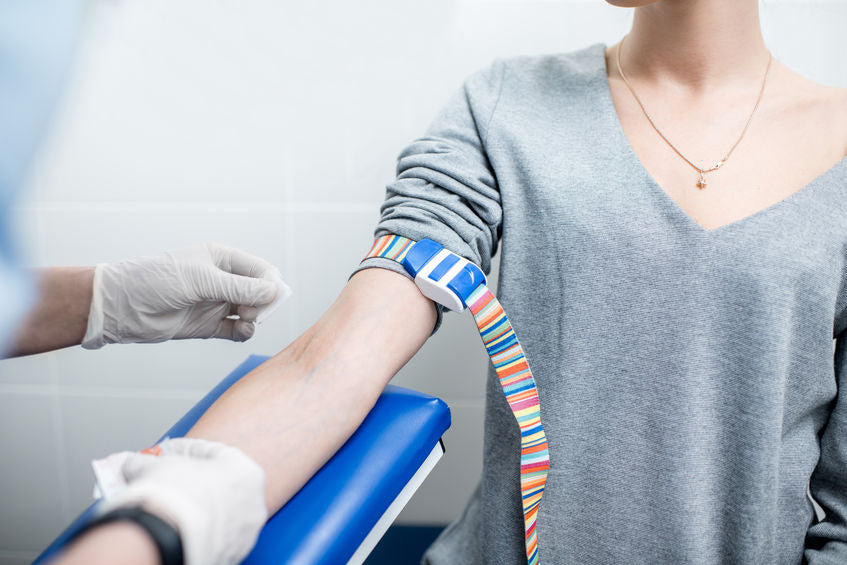
Can Blood Pregnancy Tests Be Wrong?
As a general rule, blood tests for pregnancy are more reliable than urine or home pregnancy tests. But they can be wrong. That means, they can show false negative or false positive results in some women. To understand why this can happen, we need to know what blood pregnancy tests are, how they work, and what do their results mean.
At What Point Can a Blood Test Determine Whether or Not a Woman is Pregnant?
Blood tests can detect pregnancy about 7 to 12 days after conception, making them a better option than most at home pregnancy tests. Unlike home pregnancy tests, they can also determine the level of hCG in your blood.
How Accurate is a Blood Test Compared to a Urine Test at Determining Pregnancy?
Due to recent research, it is now believed that blood tests are more accurate than urine tests when it comes to determining pregnancy accurately. According to a study from the Scientific Assembly of the American College of Emergency Physicians, about six percent of pregnancies that are reported negative from urine testing comes back positive with blood testing.
Additionally, researchers at Henry Ford Hospital examined 662 women who received both urine and blood testing for hCG. Out of the 102 negative results received, six women who tested negative with a urine test were then shown to be pregnant through blood testing. Five of the six women in this group had hCG levels ranging from 11 to 97 mU/ml, a level that appears during the first month of pregnancy.
While researchers are always wary of claiming that false negative numbers such as those reflected in the study are expected, blood pregnancy tests are now used for all women at Henry Ford Hospital who are less than four weeks past their typical menstrual period.
As a result, the conclusion can be drawn that blood tests are more accurate than urine tests at detecting pregnancy.
Blood Pregnancy Tests
A pregnancy blood test or a pregnancy serum test is a test that measures the exact amount of the pregnancy hormone, human chorionic gonadotropin (hCG), in the bloodstream.
Human chorionic gonadotropin (hCG) is a hormone that is produced by the placenta of a pregnant woman. It is detectable in the blood and urine within ten days of fertilization.
There are two types of blood pregnancy tests, namely, quantitative blood test which measures the exact amount of hCG in the blood and qualitative hCG blood test which gives a simple yes or no answer to whether you are pregnant or not.
Blood tests can detect a pregnancy earlier than a home pregnancy test (about 7-12 days from possible conception) and can also measure the concentration of hCG hormone in your blood.
The level of hCG is useful information for your healthcare provider in tracking specific problems in pregnancy. If you suspect any symptoms of pregnancy like a delayed menstrual period, breast tenderness, pelvic pain, irregular spotting or vomiting, you must get a pregnancy blood test done to confirm or rule out pregnancy.
What do the pregnancy blood test results mean?
A healthy pregnancy is expected to show a typical pattern of HCG levels over time. In a pregnant woman, the level of human chorionic gonadotropin (hCG) increases throughout the first trimester, then gradually decreases over time.
In the first trimester, a woman may have this test done repeatedly to see if the level usually rises. If it doesn't, there could be issues with the pregnancy. After childbirth, miscarriage, or abortion, the level should quickly decrease to zero.
Wrong results with blood pregnancy tests
A blood test might not detect human chorionic gonadotropin (hCG) even when a woman is pregnant if the test is done too early. It takes at least seven days after fertilization for the test to become positive. In most cases, by the time a woman has missed her period, the test will be positive if she is pregnant.
Higher than normal levels of human chorionic gonadotropin (hCG) may indicate:
- a tumor of the placenta with the death of the fetus
- multiple pregnancies, such as twins or triplets
- ovarian cancer and other types of cancer in some cases
- a normal pregnancy
- blood or protein in the urine, which can interfere with the result
- use of medications to prevent seizures, drugs to treat Parkinson's syndrome, or phenothiazine drugs, such as chlorpromazine, by the mother
- ectopic pregnancy
- a miscarriage or abortion.
How reliable are blood pregnancy tests?
Home pregnancy tests are around 97% accurate when done correctly. However, a blood test is more reliable but not necessarily more sensitive.
The results depend a lot on the lab, methodology, and technique of the blood test performed. A quantitative blood test, usually called a beta human chorionic gonadotropin (hCG) test, measures the exact units of human chorionic gonadotropin (hCG) in the blood. That means it will detect even the most minimal level.
There is another type of blood test, sometimes called a qualitative human chorionic gonadotropin (hCG) test. The qualitative pregnancy test gives a yes or no answer to whether you are pregnant. Just like home pregnancy tests, labs vary in what is considered a positive pregnancy test.
Typical cutoffs for positive blood tests for pregnancy are 5, 10, and 25 units. A level under five is considered a negative result. A blood test that is only triggered at 25 units of human chorionic gonadotropin (hCG) is not any more sensitive than several of the home pregnancy tests.
Tags:
About Pregnancy Tests
Quick links
Search
Contact Us
Shipping Information
Helpful Info
Terms of Service
Privacy Policy
Do not sell my personal information
Contact us
About us
BabyHopes.com is a family owned and operated business, opened in January 2001. We have been serving the trying to conceive community for over 20 years.

Leave a comment: