
False Positive Pregnancy Tests - What Causes Them and How Common Are They?
False positive pregnancy tests are rare - though there are instances and conditions where they can occur. Find out more here...
Tags:
About Pregnancy Tests

Marijuana Use While Trying to Conceive, Pregnant & Breastfeeding
Marijuana Use While Trying to Conceive, Pregnant & Breastfeeding - Is it safe for you and your baby? Click here to find out...
Tags:
About Pregnancy Tests
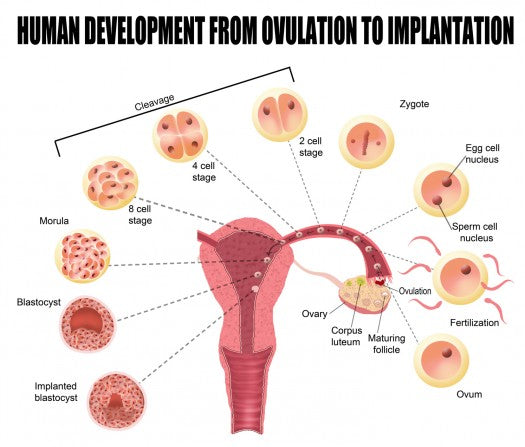
Implantation Bleeding After Conception - When it Happens & What it Looks Like
When your egg is fertilized it take a while before it implants and starts producing hCG . This article discusses how long this takes and how soon you should be able to see a positive result on a pregnancy test.
Tags:
Getting Pregnant
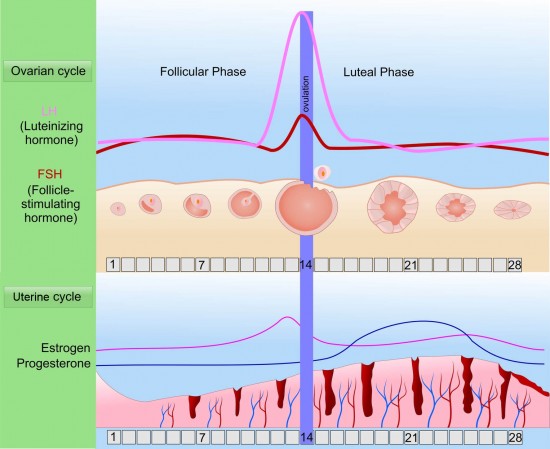
What is a Luteal Phase Defect or LPD?
What is the Luteal Phase? The luteal phase is the second part of the menstrual cycle and it is the time after ovulation until your period starts. In ideal circumstances, the luteal phase is about 14 days long but can run from 10 to 17 days long. During the luteal phase, the production of estrogen and progesterone increase. This increase helps prepare the uterine lining for the implantation of the fertilized egg. If there is no fertilization, the uterine line sheds, and your period starts. What is a Luteal Phase Defect? If the number of days between ovulation and your period starting is 10 days or less, doctors classify this as a luteal phase defect. Some doctors consider a luteal...
Tags:
Health Issues
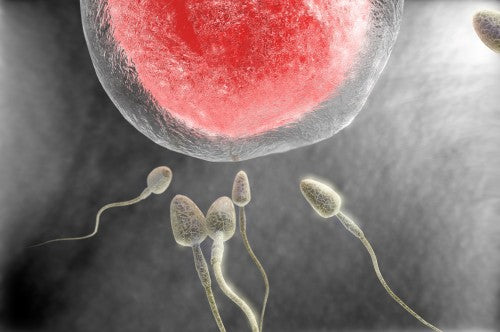
Does Abstinence Help to Improve Sperm Count?
Abstinence won't improve your chances of getting pregnant. Studies have shown that men with normal sperm count and motility can go a bit over a week without ejaculation, and sperm health doesn't suffer. If you have sperm health issues, you should only abstain for a day for the best quality sperm. Additionally, if you abstain for too long, you could cause harm to your sperm. The motility and morphology of your sperm will deteriorate if you abstain for over a week. As you might suspect, this is extremely damaging when it comes to conception. Thus, the studies state that men should ejaculate between three and four times a week to ensure proper motile, healthy sperm. A...
Tags:
About Sperm
How Long Can Sperm Live Inside The Female Body?
This post contains affiliate links. We will earn a small commission if you purchase something after clicking on the link. Read our affiliate disclosure here. How Long Alright, ladies, let's get personal. We're going to talk about sperm. Sperm is a vital part of the journey when you make the official "try to conceive" decision. We all know that ovulation is necessary to get pregnant, but sperm plays an equally important role. Women know their bodies intimately when tracking fertility but may overlook the sperm aspect. It's essential to know how long sperm can live inside the female body to optimize your chances of getting pregnant. Does Sperm Survive After Ejaculation? Your body is close to the temperature...
Tags:
About Sperm

How To Get Pregnant - 9 Tips To Help You Conceive
This post contains affiliate links. We will earn a small commission if you purchase something after clicking on the link. Read our affiliate disclosure here. You'd think most people would know how to get pregnant, but many couples find out that it isn't as easy as just having sex. Many things can make getting pregnant harder than you expected. If you choose to follow the advice, these nine tips can help increase your chances of getting pregnant. What You Should Start Doing - Fertility Friendly Habits 1) Most Important How To Get Pregnant Tip - Know When You Ovulate! Knowing when you ovulate is one of the biggest things you can do to help improve your chances...
Tags:
Getting Pregnant
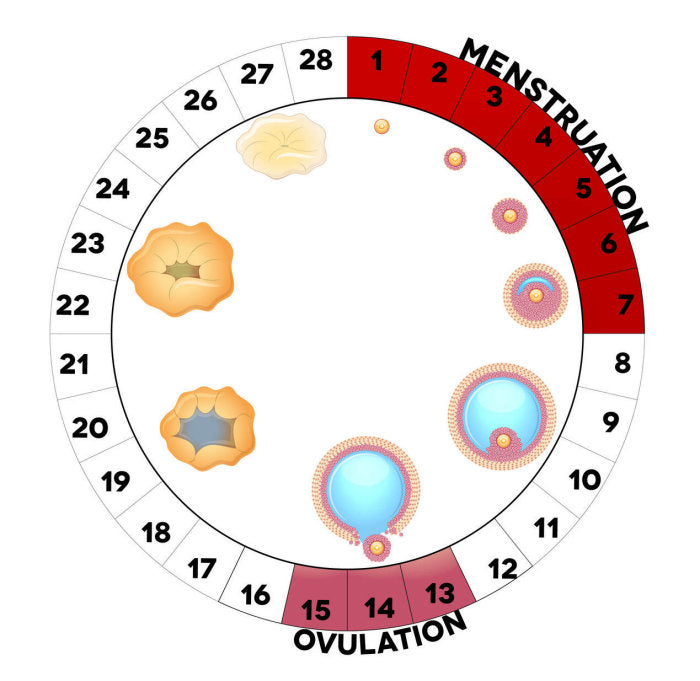
Why Is My Ovulation Test Positive For 2 Days In a Row?
This post contains affiliate links. We will earn a small commission if you purchase something after clicking on the link. Read our affiliate disclosure here. Identifying when you are most fertile is essential for timing intercourse for getting pregnant. Many women become stressed when trying to determine their most fertile days. The stress increases when they get a positive ovulation test 2 days in a row. They become worried that if they do not time intercourse just right, their chances of getting pregnant are small. While this is true, there are ways to track your fertility to better time having sex. One of those ways is to use an ovulation predictor kit or test, often referred to as...
Tags:
Ovulation
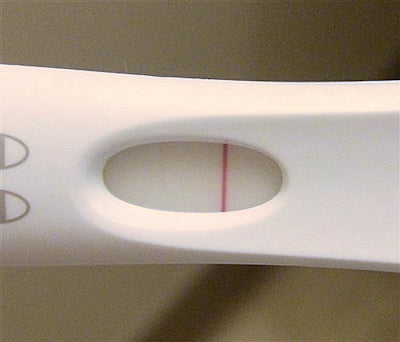
Evaporation Lines and Early Pregnancy Tests
What are Pregnancy Test Evaporation Lines? As the name suggests, evaporation lines appear due to urine evaporation within the testing area of your pregnancy test. These lines show up in the result window of the test, exactly where a positive sign would be. An evaporation line develops when the urine on the test area begins to dry, leaving a faint line. What Causes Evaporation Lines on a Pregnancy Test? These lines show up due to the particular urine specimen's composition and may appear on any test regardless of brand. You may see a clear-ish line if you read the results after the time frame the instructions stated or if you took the test incorrectly. How Common are They? Evaporation...
Tags:
About Pregnancy Tests

Does Sperm Count Decrease As You Get Older?
Men also have a biological clock – they too experience a natural decline in their testosterone levels as they age. This causes a decrease in their sex drive and energy levels, and makes it difficult for them to achieve and maintain an erection. Men's Biological Clock According to Dr. Harry Fisch, the author of "The Male Biological Clock", male infertility increases with age, along with a decline in testosterone levels, and decreased sperm quality .Older men are more likely to father children with a significant genetic abnormality than younger men. This genetic abnormality arises in the babies that are born of the sperm of older men. As with women, men's biological clocks also start ticking around the age of thirty...
Tags:
About Sperm
Quick links
Search
Contact Us
Shipping Information
Helpful Info
Terms of Service
Privacy Policy
Do not sell my personal information
Contact us
About us
BabyHopes.com is a family owned and operated business, opened in January 2001. We have been serving the trying to conceive community for over 20 years.
